Insulin pump & CSLC CAP

Insulin pump & CSLC CAP
- Binoy
- March 21, 2019
- 0 Comments
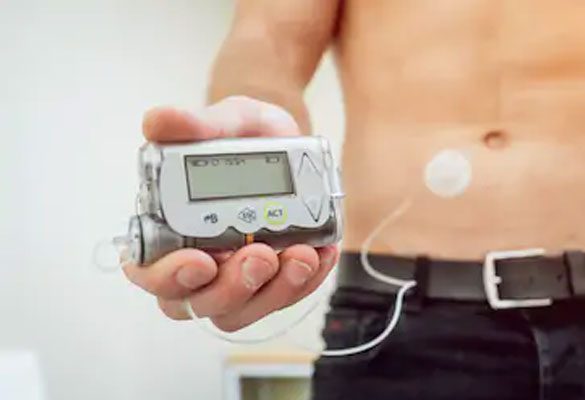
An insulin pump is a small computerized device that delivers insulin throughout the day for the treatment of diabetes. Insulin pump provides continuous delivery of short acting insulin all day long in diabetic patients. It appears to mimic the pancreas but you still have to monitor your glucose level and give it instructions for the correct amount of insulin to be released.
It releases insulin in two ways: a basal rate where a small continuous quantity of insulin is released in between meals and overnight to keep a constant glucose level in the body and a bolus rate where much higher insulin is released before meals to control the glucose release from the food you plan to eat.
The basal insulin rates are usually set up in your pump with your doctor, and you can have one or multiple basal settings programmed in your pump, based on your needs. You program the amount of insulin for your mealtime bolus directly on the pump. Most pumps come with built-in bolus calculators to help you figure out how much insulin you need at mealtime based on your glucose levels and the amount of carbohydrates you are eating. Thus an insulin pump replaces the need for multiple daily injections.
The pump, which is about the size of a smartphone, is worn on the outside of your body and delivers insulin through a tube (catheter), connected to a thin cannula, placed into the layer of fat under your skin, typically around your stomach area.
To use an insulin pump, you will need hands-on training from your diabetes care team. They will teach you how to fill a pump reservoir, prime tubing, select an infusion site, change an infusion set, disconnect the device, calculate and program basal and bolus doses, troubleshoot potential problems, create backup plans in case of pump failure, and prevent diabetic ketoacidosis.
Advantages Of Insulin Pumps includes:
- Fewer needle pricks: The pumps require a needle stick every 2-3 days in comparison to the multiple pricks in a single day from insulin injections.
- Precision: They allow accurate delivery of insulin to the 1/10th that is beneficial to people sensitive to small doses, like children.
- Dose calculations: Pumps have a calculator that saves the user from the extra math by helping to determine the doses based on the carb intake, blood glucose levels and the amount of insulin still active from the previous doses.
- Flexibility, convenience, and spontaneity: They allow easy adjustments with buttons to either increase or decrease the bolus for accommodating the changes in daily life like dining out, sports, growth, and illness or managing the dawn phenomenon (drop in glucose levels at night time).
- Eliminates unpredictable effects of long-acting insulin-They use rapid-acting insulin that has an efficient action for a short duration instead of intermediate or slow acting insulin that take a while to reach their peak values and tend to accumulate under the skin which makes it difficult to predict the action of insulin.
- Reduced episodes of severe low blood sugar: By using rapid-acting insulin and allowing better control of released insulin during or before activities that tend to lower blood glucose, you have less risk of having a hypoglycemic attack.
- Pumps improve A1C scores and less glucose variability (high to low or low high swings).
Disadvantages Of Insulin Pumps include:
- Cost: Insulin pumps are more expensive than the syringes.
- Steep learning curve: It takes a few days for the user to get used to changing infusion sets, getting the basal and bolus doses regulated and learning to avoid problems like bubbles.
- Complication: A higher risk of developing diabetic ketoacidosis if the pump malfunctions. This can happen if the battery is discharged, if the insulin is inactivated by heat exposure, if the reservoir runs out, if the tubing becomes loose there is a leak of insulin or the catheter is bent or kinked preventing delivery. Therefore, it is important for pump users to monitor their blood glucose levels frequently.
- Inconvenience: Since the pumps need to be worn all the time, it can become an issue during sleep, rough sports or doing activities like swimming. The tubing can also get caught on hooks.
- Skin problems: Users develop scar tissue in the area where the cannula is inserted. These scar tissues do not heal easily and soon develop lower insulin sensitivity that requires the user to change spots. A patient may run out of viable spots to wear the pump. The user may also experience skin irritation in the area where the pump is inserted.
- Changing issues: Although the pump requires a change at every two-three days, the process is longer, more involved.
- Wastage: Many units of insulin can be wasted while refilling the reservoir or changing the infusion site. This can affect dosage information.
Conclusion
In type 2 diabetes there is no insulin deficiency and insulin resistance induced hyperglycemia can be controlled within days with clinically monitored lifestyle optimization with Cell Activation Support Care. HbA1c values can be brought down to non diabetic levels within 3 to 4 months even in severely diabetic patients with HbA1c more than 10. So there is no need to consider a complicated and expensive device like insulin pump in type 2 diabetes or even insulin injection with the development of cell activation treatment.
